Achilles Tendon Pain in Runners: Causes, Fixes, and Prevention
- Felicia Sciortino

- Aug 28, 2025
- 4 min read

As a runner, few things are more frustrating than that nagging stiffness in the back of your ankle that shows up during or after a run. Achilles tendon pain—also called Achilles tendinopathy—is one of the most common overuse injuries I see in runners. It’s stubborn, it lingers, and if ignored, it can sideline you for months.
The good news? With the right strategies, you can not only recover from Achilles pain but also build resilience so it doesn’t keep coming back.
Understanding Achilles Tendinopathy
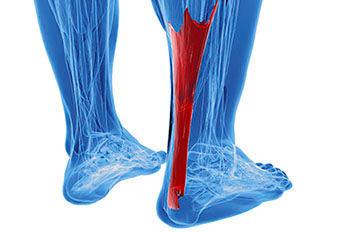
Your Achilles tendon connects your calf muscles (the gastrocnemius and soleus) to your heel bone. Every step you take, it stores and releases energy—like a spring—to propel you forward. That means it takes on a lot of repeated stress during running.
Achilles tendinopathy usually presents as:
Stiffness in the morning or at the start of a run
Pain that eases once you “warm up,” then returns after activity
Tenderness at the back of the heel or just above it
The Role of Heel-to-Toe Drop in Running Shoes

One shoe feature that has a direct impact on the Achilles is heel-to-toe drop—the difference in height between the heel and the forefoot.
High drop shoes (8–12mm): These slightly elevate the heel, reducing how much the Achilles has to lengthen with each step. This can decrease tendon strain, making them useful during flare-ups.
Low drop shoes (0–4mm): These increase the demand on the Achilles by requiring more dorsiflexion (ankle bend) and tendon stretch. Great for building durability if you progress slowly—but a fast switch into low-drop shoes can overload the tendon.
Bottom line: heel drop should be a tool, not just a preference. Rotating shoes with different drops strategically can help manage stress while still building tendon resilience over time.
Heel Lifts: A Helpful Short-Term Strategy
In some cases, adding a small heel lift insert inside your shoe can provide short-term relief. By slightly raising the heel, the lift reduces tension on the Achilles, giving the tendon a chance to calm down while you keep moving.
Important note: heel lifts aren’t a long-term fix. They should be used as a temporary aid alongside a structured strength program. Once symptoms improve, the goal is to gradually wean off the lift so the tendon regains its full capacity.
Manual Therapy Options

While exercise and load management are the foundation of Achilles rehab, certain manual therapy techniques can provide short-term relief and help you move forward with your training.
Dry Needling: Targeting the calf muscles with dry needling can reduce muscle tension, improve blood flow, and decrease pain, making it easier to perform your rehab exercises.
Soft Tissue Mobilization: Hands-on techniques like massage or instrument-assisted soft tissue mobilization (IASTM) can help improve tissue quality around the calf and Achilles, reducing stiffness.
Joint Mobilization: Improving ankle mobility (especially dorsiflexion) can decrease compensations that otherwise overload the tendon.
These strategies don’t “fix” the tendon on their own—but they can make the rehab process smoother by calming pain, restoring motion, and setting you up for success with strength training.
Why Heavy Strength Training is Non-Negotiable
Here’s the thing—tendons don’t respond the same way muscles do. Light resistance, high reps, or endless bodyweight calf raises won’t cut it for Achilles rehab or prevention.
To build a stronger, more resilient tendon, you need heavy, slow, controlled loading. Think:
Straight-leg calf raises (targets gastrocnemius)
Bent-knee calf raises/seated calf raises (targets soleus)
Progression from double-leg → single-leg → weighted variations
And here’s a critical point: it’s safe to work through mild levels of pain (usually 2–3/10 on a pain scale) during this type of training. Completely avoiding discomfort often means you’re under loading the tendon, which slows or even prevents tendon repair. The goal is to load the tendon enough to stimulate adaptation—without pushing into sharp or lingering pain.

Progressing to Plyometrics
Once symptoms have calmed down and your strength work feels solid, the next step is plyometric training. This is where you rebuild the tendon’s ability to store and release energy—exactly what it does when you run.
Key progressions include:
Double-leg hops → single-leg hops
Skipping drills
Bounding or power-focused jumps
Short bouts of uphill sprints
These should be added gradually and layered on top of a foundation of heavy strength training. Think of them as the bridge between rehab exercises and a full return to pain-free, powerful running.
Putting It All Together
Manage training load: Avoid sudden mileage spikes or abrupt changes in terrain.
Use heel-to-toe drop strategically: Higher drop shoes or a temporary heel lift can help in the short term, but long-term resilience comes from gradually loading the tendon.
Incorporate manual therapy as needed: Techniques like dry needling or soft tissue work can reduce pain and stiffness, making it easier to stay consistent with your program.
Prioritize heavy strength work: Load the tendon with slow, heavy resistance—even if there’s mild discomfort.
Progress to plyometrics: Restore the tendon’s spring-like function to truly return to performance.
Take Control of Your Running Health
Achilles tendon pain doesn’t have to derail your training. By combining smart shoe choices, short-term strategies like heel lifts, manual therapy for symptom relief, heavy strength training, and progressive plyometric work, you can not only get past the pain but build a tendon that’s more resilient than ever.
If you’re struggling with Achilles pain—or want to make sure it doesn’t show up during your marathon training—schedule a free consult and let’s build a plan tailored to you.



Comments